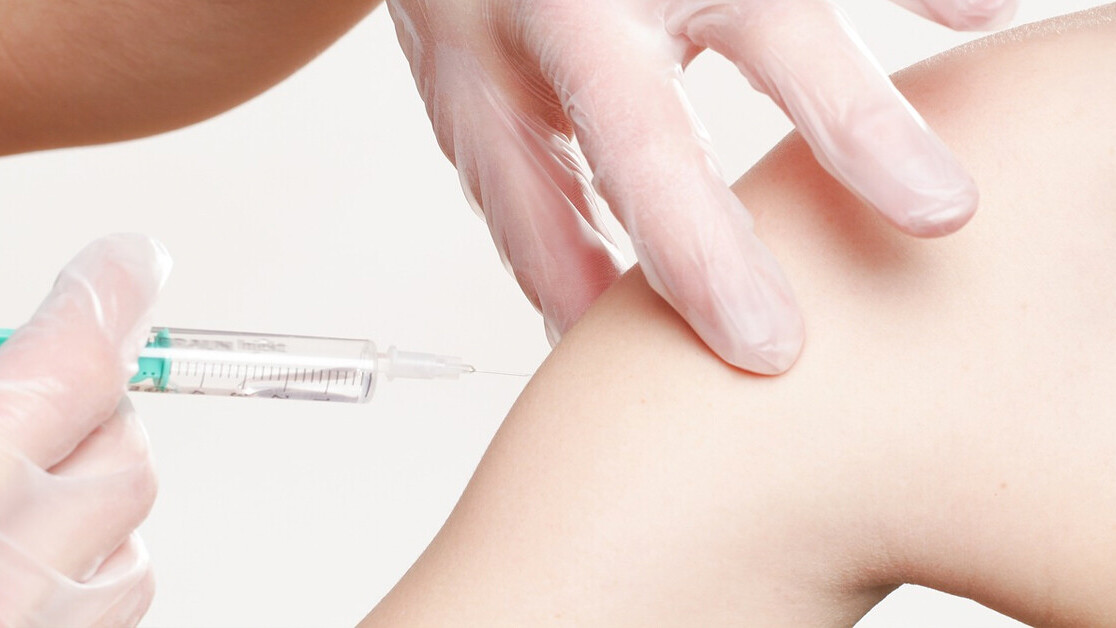
Donald Trump may be “very confident” we will have a vaccine for COVID-19 by the end of the year, but the rest of us should be more cautious. Billions of dollars are being spent trying to develop vaccines and treatments as a more permanent solution to the crisis than the lockdowns currently being enforced around the world.
As of May 2020 there are 182 treatments and 99 different vaccines being developed globally. But, based on recent history, only one or two are likely to be transformative, a couple may be partially helpful, some will be shown as downright dangerous, and the majority will have conflicting evidence as to their effectiveness.
This is because medical research is a slow and painstaking process. It is also very complicated and easy to come to the wrong conclusions.
Trusting the experts
One good thing to have come out of the coronavirus pandemic seems to be a renewed trust in experts. The routine presence of scientists at government briefings seems to recognize that rather than deserving our suspicion, we need these people to beat the virus.
But more trust in experts means more scrutiny of science as it happens – the latest studies showing promising results are now headline news. This can be worrying because, while there is no doubt that treatments for COVID-19 will eventually be found, it is easy for enthusiasm to turn into cynicism if expectations are not met as quickly as the public and politicians may hope.
Read: [Will a coronavirus vaccine change the minds of anti-vaxxers?]
There seems to be little recognition that, while thousands of drugs have shown promise in early animal or clinical tests – for example, the vaccine trials at the University of Oxford – the vast majority that show early promise will never make it into routine clinical use. On average it takes 12 years and over US$1 billion (£805 million) to get a drug to market.
Good research takes time
I chair research ethics committees. Over the last few years I have reviewed thousands of research protocols representing the very best, and occasionally some quite poor, examples of medical research.
Good research is defined as rigorous and reliable, producing results that are not only interesting but are practical, useful, and in some cases transformative. They are also reported clearly, transparently, and in the context of previous studies. This is precisely the type of research we need to address the COVID-19 crisis.
But such good research comes at a cost. Much of society think of the cost in terms of dollars and pounds, and indeed mindful of our own survival, scientists and researchers are of course always going to lobby for more investment. While it is very helpful to have the funds to order any chemical that is needed, access highly specialized equipment, or pay others to conduct experiments and analyze results quickly, we must take care never to underestimate the importance of taking time to think carefully about what results actually mean.
It is only once researchers have taken the time to understand the context of results that they can start turning them into effective applications or treatments. The real cost of good research is therefore time.
The frustrating truth about medical research is that the majority of experiments appear not to work because the subject being studied is so horrendously complex. In fact, rather than “not working,” many experiments are simply inconclusive. To make progress you have to slow down, look at the evidence , and take time to think very carefully about what the results might mean.
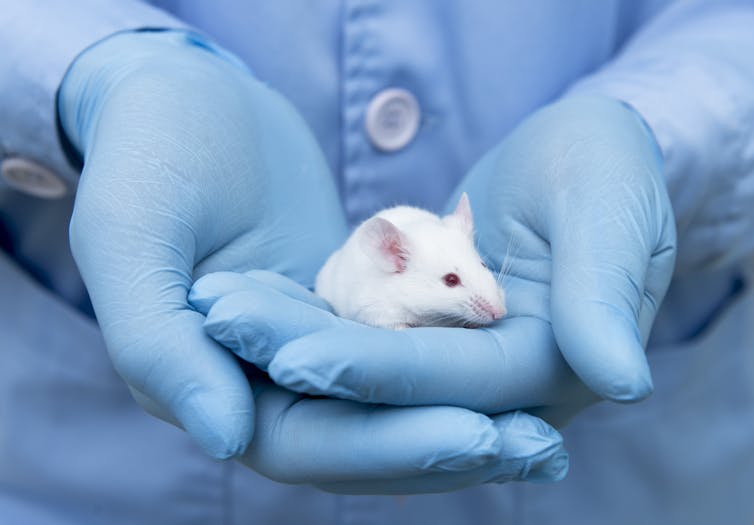
The thinking needed for this takes years. I was involved with one project that was delayed for almost ten years while the team tried to work out why a single animal showed cardiovascular complications. Another project I worked on showed promise reducing an Alzheimer-like pathology in mice, yet 18 years later similar effects have yet to be conclusively shown in humans. Commendably, the team is still working on it.
The reality is that the long road to a vaccine or drug for any disease is littered with trials that did not lead to expected results. Even when a study is successful, it takes a long time to go from the lab to the general public.
The pressure to find a cure
One worrying aspect of the current situation is the pressure on researchers to work quickly and come up with solutions for COVID-19 almost immediately. For perhaps the first time, financial resources are not a limiting factor, and so politicians and the public are expecting researchers to take the cash and provide the answers. This has been coupled with significant pressure on regulators to streamline or even suspend some of the normal processes so that treatments can get to the clinic as quickly as possible.
Lured by promises of unlimited funding, and perhaps fame should their chosen idea work, some researchers may be tempted to engage in questionable research practices. History shows that whenever a large amount of money is involved, the temptation to commit, fraud, misconduct, or other questionable practices increase. The UK spent more than £400 million during the 2009 swine flu outbreak stockpiling a drug whose effectiveness had been inflated by the manufacturers due to publication bias – where negative or inconclusive results from a trial are not published in scientific journals, but positive results are.
Without appropriate scrutiny, there is a real risk that ineffective, or even harmful, treatments begin to get used. This may be considered an acceptable risk in the current crisis, but if so, it is important that any new treatments are monitored very closely and withdrawn without hesitation if the harms mount up.
Given time – maybe two, three or perhaps even ten years – researchers will be able to take stock of the evidence from experiments and trials, perform a meta-analysis and systematic review, hold international conferences, and then, following careful thought, tell the world what the best treatment for COVID-19 is.
The world clearly needs scientific and medical answers to the current pandemic as soon as possible, but we need to recognize that initially, we may only find partial or tentative answers. Instead of a quick vaccine that completely prevents COVID-19, a variety of partial successes will be combined until eventually a full solution is found.
There may even be some blind alleys with promising, but ultimately futile, treatment ideas. This is not a failure of research, or misuse of resources. Above all, researchers need to be supported to work with integrity, and not be made scapegoats for the challenges that undoubtedly lie ahead.![]()
This article is republished from The Conversation by Simon Kolstoe, Senior Lecturer in Evidence Based Healthcare and University Ethics Advisor, University of Portsmouth under a Creative Commons license. Read the original article.
Get the TNW newsletter
Get the most important tech news in your inbox each week.